A neuroscientist explains the glymphatic system; evolution’s answer to brain waste that no supplement can replicate
The wellness industry desperately wants to sell you a brain detox. Activated charcoal smoothies. Heavy metal cleanses. Infrared sauna sessions. The promises are seductive: flush toxins from your brain, restore mental clarity, prevent cognitive decline.
Here’s what they won’t tell you: your brain already has a detoxification system. It’s called the glymphatic system, it was only discovered in 2012, and it does something no juice cleanse ever could. It physically flushes metabolic waste from your brain tissue at speeds far faster than diffusion alone could manage. The catch? It operates almost exclusively while you sleep. And the modern world is systematically preventing it from working.
I find this discovery genuinely thrilling. We’ve spent decades searching for ways to clear the toxic proteins associated with Alzheimer’s and Parkinson’s disease. Turns out evolution solved this problem long ago. We just hadn’t noticed. The real question now isn’t how to detox your brain, it’s how to stop sabotaging the system you already have.
The Discovery Nobody Expected
For most of medical history, neuroscientists assumed the brain simply didn’t need the kind of waste-removal system that exists throughout the rest of your body. The lymphatic system, that network of vessels that clears dead cells and debris from your tissues, was thought to stop at the blood-brain barrier. The brain, we believed, handled its own cleanup through slow diffusion and local degradation.
We were wrong.
In 2012, a lab at the University of Rochester used two-photon microscopy to watch cerebrospinal fluid flow through the brains of living mice (1). What they saw was remarkable: a network of channels running alongside blood vessels, rapidly flushing waste products from brain tissue. They called it the “glymphatic” system, a nod to its dependence on glial cells and its functional similarity to the lymphatic system elsewhere in your body.
The basic mechanism works like this: cerebrospinal fluid flows into your brain along the spaces surrounding arteries, then gets pumped through brain tissue by specialized water channels (called aquaporin-4 or AQP4) on the end-feet of astrocytes, star-shaped support cells that wrap around your blood vessels. This flow mixes with interstitial fluid (the fluid your cells float in), picking up metabolic waste, then drains out along veins and eventually into your lymphatic system for disposal (2).

(Figure: Schematic of the glymphatic system. Graphic made using Biorender.)
This isn’t a gentle trickle. It’s a pressure-driven flush that clears waste far more efficiently than passive diffusion. And here’s what’s critical: this system is approximately 90% more active during sleep than wakefulness (3).
Why Your Brain Only Cleans Itself When You Sleep
This is where things get genuinely surprising. In 2013, Nedergaard’s team published a landmark paper in Science showing that the interstitial space in mouse brains expands by approximately 60% during sleep (4). This expansion allows cerebrospinal fluid to flow more freely through brain tissue, dramatically increasing waste clearance.
Think about that for a moment. Your brain cells physically shrink while you sleep, creating more space between them for cleaning fluid to flow through. It’s like your neurons are collectively exhaling, making room for the night shift to come through with mops and buckets.
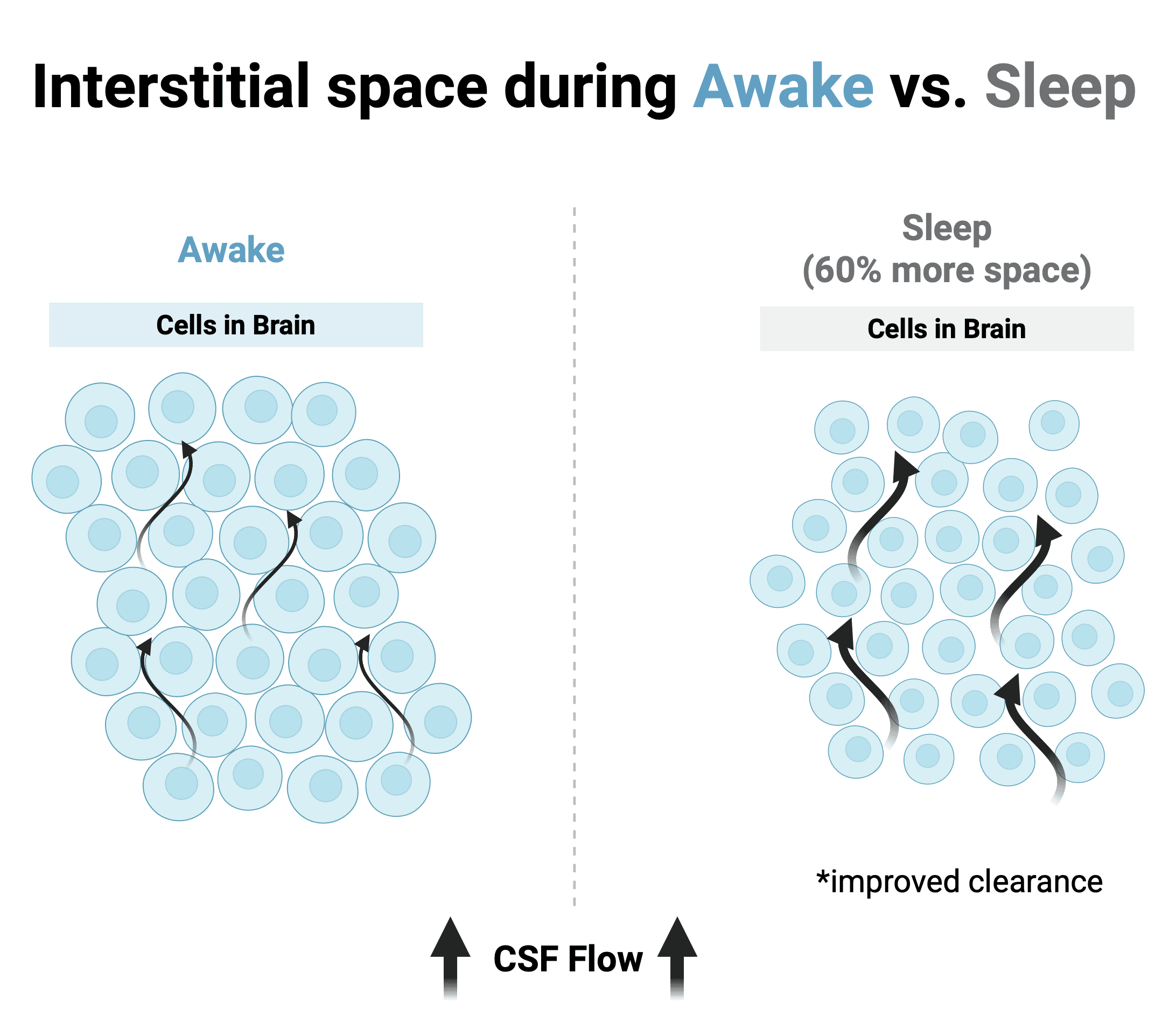
(Figure: Interstitial space between cells in the brain increases by 60% during sleep, allowing for more efficient clearance of debris/waste. Graphic made with Biorender.)
The mechanisms are now better understood. During non-rapid-eye-movement (NREM) sleep, particularly the deep N3 stage characterized by slow oscillatory brain waves, several things happen simultaneously:
- Norepinephrine levels drop, causing blood vessels to dilate and reducing resistance to fluid flow
- The slow rhythmic waves of deep sleep create physical pulsations that help pump fluid through the system
- The interstitial space expands, creating channels for waste removal
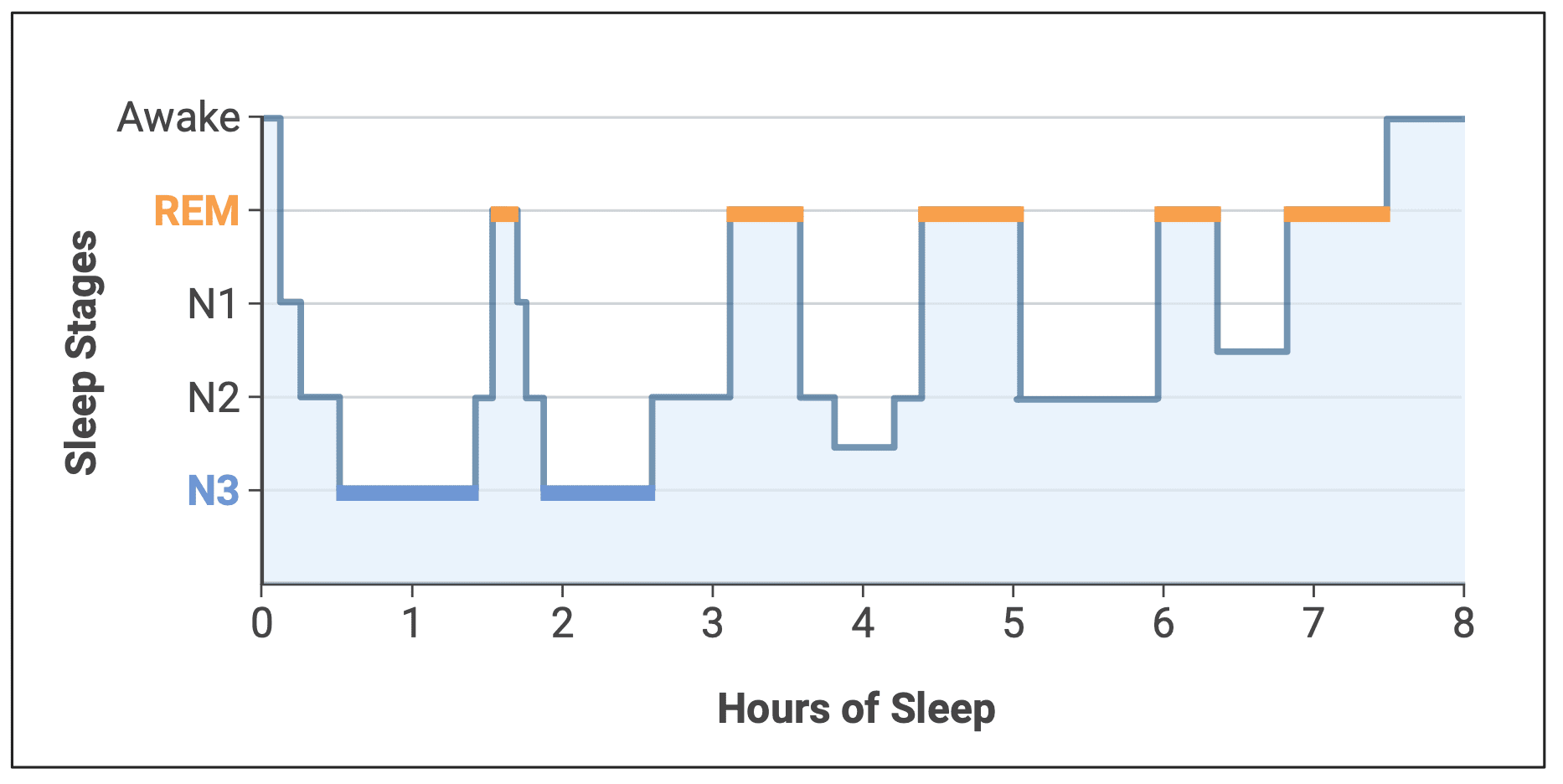
(Figure: Stages of sleep. Graphic made using Biorender.)
A January 2025 study in Cell added crucial detail: rhythmic oscillations in norepinephrine during NREM sleep coordinate with blood vessel diameter changes to drive glymphatic flow (5). When researchers gave mice zolpidem (Ambien), it suppressed these oscillations and reduced glymphatic clearance.
The implication is striking: sleeping pills might make you unconscious without giving your brain the cleaning it needs. Sedation isn’t sleep. Your brain knows the difference.
The Toxic Proteins That Accumulate When the System Fails
The glymphatic system clears exactly the proteins we associate with neurodegenerative disease.
Amyloid-beta, the protein that forms the plaques characteristic of Alzheimer’s disease, is cleared via glymphatic pathways (6). So is tau, the protein that forms neurofibrillary tangles. In Alzheimer’s mouse models, researchers have shown that impairing glymphatic function accelerates both amyloid and tau accumulation (7).
Alpha-synuclein, the protein that aggregates in Parkinson’s disease, also appears to be cleared through this system (8). When researchers blocked meningeal lymphatic drainage in Parkinson’s model mice, alpha-synuclein accumulated, dopaminergic neurons died, and motor dysfunction followed.
The evidence in humans is mounting. A 2017 study published in JAMA Neurology examined post-mortem brain tissue and found that loss of AQP4 polarization, meaning the water channels that drive glymphatic flow were no longer properly positioned, was significantly greater in Alzheimer’s patients than controls (9). More troubling: this depolarization correlated with the APOE ε4 gene variant, the strongest genetic risk factor for Alzheimer’s.
Even a single night of sleep deprivation increases amyloid-beta levels in human brains, as shown by PET imaging (10). Your brain is literally dirtier after pulling an all-nighter.
What Damages the System
Several factors impair glymphatic function, and none of them can be fixed by a supplement.
Aging: This is the big one. A foundational 2014 study showed that glymphatic function declines dramatically with age (11). Compared to young mice, old mice showed 40% reduced clearance of amyloid-beta from the brain. The mechanism involves loss of AQP4 polarization, the water channels become scattered across astrocyte cell bodies rather than concentrated at blood vessel contact points, combined with reduced arterial pulsatility that normally helps pump cerebrospinal fluid.
Sleep disruption: Chronic sleep problems, including obstructive sleep apnea, are associated with reduced glymphatic function and accelerated Alzheimer’s pathology. It’s not just total sleep time that matters, it’s the architecture of your sleep. Fragmented sleep with frequent awakenings may prevent the sustained deep sleep states necessary for efficient clearance.
Head trauma: After traumatic brain injury, AQP4 becomes dislocated from its normal position at astrocyte end-feet, impairing glymphatic flow (12). This may help explain why repeated concussions are associated with later neurodegeneration.
Chronic inflammation: Neuroinflammation impairs glymphatic function, and glymphatic impairment worsens neuroinflammation creating a potential vicious cycle (13).
Notice what’s not on this list: toxin exposure from non-organic produce, heavy metals from dental fillings, or whatever else the wellness industry is blaming this week. The real threats to your brain’s cleaning system are far more mundane and far more under your control.
The Human Evidence Is Now Confirmed
For years, skeptics argued that the glymphatic system was a rodent curiosity that might not exist in human brains. That critique died in October 2024.
Researchers at Oregon Health & Science University published the first direct visualization of glymphatic flow in living humans (14). They injected a tracer into the cerebrospinal fluid of five patients undergoing brain surgery, then tracked its movement with MRI. The images showed cerebrospinal fluid flowing along perivascular spaces in clearly defined channels, exactly as predicted by the glymphatic hypothesis.
What Actually Helps (And It’s Not a Cleanse)
The factors that improve glymphatic function are frustratingly simple and can’t be bottled and sold.
Sleep quality matters more than duration: Deep NREM sleep is when glymphatic clearance peaks. Factors that increase deep sleep, regular sleep schedules, cool bedroom temperatures, and limiting alcohol likely support brain clearance. Interestingly, sleep position may matter: lateral sleeping appears more efficient for glymphatic clearance than supine (back) or prone (stomach) positions (15).
Exercise: A 2025 study in Nature Communications provided the first human evidence that physical exercise enhances glymphatic function (16). Twelve weeks of regular cycling significantly increased both glymphatic influx and meningeal lymphatic vessel flow in healthy volunteers. The researchers also found that exercise reduced inflammation-related proteins in blood plasma potentially explaining the mechanism.
Animal studies have shown that voluntary exercise increases AQP4 expression, improves its localization at astrocyte end-feet, accelerates amyloid clearance, and reduces neuroinflammation (17).
Not much else has strong evidence: Intermittent fasting shows some promise in animal models for improving AQP4 polarization (18), but human data is limited. Various drugs are being investigated, but nothing is ready for clinical use.
The wellness industry hates this. They can’t sell you sleep. They can’t monetize a jog around the block. But evolution didn’t design your brain’s cleaning system to require expensive interventions. It designed it to run automatically. If you let it.
The Bigger Picture
The glymphatic hypothesis offers something the dementia field has desperately needed: a unifying framework. Sleep disruption, aging, head trauma, cardiovascular disease, all known risk factors for Alzheimer’s, converge on glymphatic dysfunction (19).
This doesn’t mean glymphatic failure causes Alzheimer’s. The relationship is almost certainly bidirectional: toxic protein accumulation can impair glymphatic function, which allows more accumulation, which causes more impairment. Breaking this cycle at any point might slow disease progression.
Clinical trials are already underway testing whether enhancing glymphatic function can prevent or slow neurodegenerative disease. The approaches range from pharmacological (drugs that promote deep sleep or improve AQP4 function) to behavioral (exercise programs, sleep optimization).
But the most important implication might be the simplest: we’ve been searching for ways to clear toxic proteins from the brain while systematically destroying the system evolution built for exactly that purpose. Every late night, every disrupted sleep cycle, every year of chronic sleep deprivation. We’re not just tired. We’re dirty.
The Bottom Line
Your brain has a sewage system. It evolved over millions of years. It runs almost exclusively during deep sleep. When it fails from aging, sleep deprivation, or chronic inflammation, toxic proteins accumulate. This may be the final common pathway to dementia.
No supplement can replicate what evolution built. No cleanse can substitute for sleep. The real brain detox isn’t something you buy, it’s something you allow to happen by getting out of its way.
The science is clear. The hard part is behavior change in a world that treats sleep as optional and rest as laziness. That “I’ll sleep when I’m dead” line? It will definitely come quicker if you neglect sleep. Your brain cleans itself every night. The question is whether you’re giving it the chance.
Stay Curious,
Andrew

References
- Iliff JJ, Wang M, Liao Y, et al. A paravascular pathway facilitates CSF flow through the brain parenchyma and the clearance of interstitial solutes, including amyloid β. Science Translational Medicine. 2012;4(147):147ra111.
- Jessen NA, Munk ASF, Lundgaard I, Nedergaard M. The glymphatic system: a beginner’s guide. Neurochemical Research. 2015;40(12):2583-2599.
- Benveniste H, Liu X, Koundal S, et al. The glymphatic system and waste clearance with brain aging: a review. Gerontology. 2019;65(2):106-119.
- Xie L, Kang H, Xu Q, et al. Sleep drives metabolite clearance from the adult brain. Science. 2013;342(6156):373-377.
- Hauglund NL, Pavan C, Nedergaard M. Norepinephrine-mediated slow vasomotion drives glymphatic clearance during sleep. Cell. 2025;188(1):137-151.
- Harrison IF, Ismail O, Machhada A, et al. Impaired glymphatic function and clearance of tau in an Alzheimer’s disease model. Brain. 2020;143(8):2576-2593.
- Iliff JJ, Chen MJ, Plog BA, et al. Impairment of glymphatic pathway function promotes tau pathology after traumatic brain injury. Journal of Neuroscience. 2014;34(49):16180-16193.
- Zou W, Pu T, Feng W, et al. Blocking meningeal lymphatic drainage aggravates Parkinson’s disease-like pathology in mice overexpressing mutated α-synuclein. Translational Neurodegeneration. 2019;8:7.
- Zeppenfeld DM, Simon M, Haswell JD, et al. Association of perivascular localization of aquaporin-4 with cognition and Alzheimer disease in aging brains. JAMA Neurology. 2017;74(1):91-99.
- Shokri-Kojori E, Wang GJ, Wiers CE, et al. β-Amyloid accumulation in the human brain after one night of sleep deprivation. Proceedings of the National Academy of Sciences. 2018;115(17):4483-4488.
- Kress BT, Iliff JJ, Xia M, et al. Impairment of paravascular clearance pathways in the aging brain. Annals of Neurology. 2014;76(6):845-861.
- Ren Z, Iliff JJ, Yang L, et al. ‘Hit & Run’ model of closed-skull traumatic brain injury (TBI) reveals complex patterns of post-traumatic AQP4 dysregulation. Journal of Cerebral Blood Flow & Metabolism. 2013;33(6):834-845.
- Nedergaard M, Goldman SA. Glymphatic failure as a final common pathway to dementia. Science. 2020;370(6512):50-56.
- Yamamoto EA, Bagley JH, Geltzeiler M, et al. The perivascular space is a conduit for cerebrospinal fluid flow in humans: A proof-of-principle report. Proceedings of the National Academy of Sciences. 2024;121(42):e2407246121.
- Lee H, Xie L, Yu M, et al. The effect of body posture on brain glymphatic transport. Journal of Neuroscience. 2015;35(31):11034-11044.
- Kim YK, Nam KI, Song J. Long-term physical exercise facilitates putative glymphatic and meningeal lymphatic vessel flow in humans. Nature Communications. 2025;16:3315.
- He XF, Liu DX, Zhang Q, et al. Voluntary exercise promotes glymphatic clearance of amyloid beta and reduces the activation of astrocytes and microglia in aged mice. Frontiers in Molecular Neuroscience. 2017;10:144.
- Reddy OC, van der Werf YD. The sleeping brain: harnessing the power of the glymphatic system through lifestyle choices. Brain Sciences. 2020;10(11):868.
- Rasmussen MK, Mestre H, Bhargav N. The glymphatic pathway in neurological disorders. The Lancet Neurology. 2018;17(11):1016-1024.

Leave a Reply